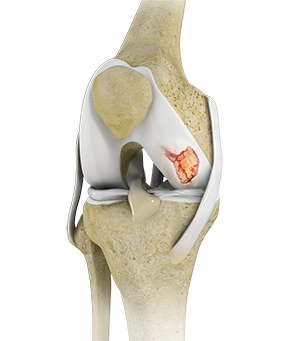
What is Knee Cartilage Restoration?
Knee cartilage restoration is a surgical technique to repair damaged articular cartilage in the knee joint by stimulating new growth of cartilage or by transplanting cartilage into areas with defects in order to relieve pain and restore normal function to the knee.
Articular cartilage damage can occur from normal wear and tear of the knee joints, increasing age, injury, or other disease conditions. When cartilage is damaged, it can cause severe pain, inflammation, stiffness, and decreased range of motion of the knee. Because of its avascular nature (absence of blood supply), cartilage cannot repair itself and therefore surgical treatment is usually required to restore cartilage function and prevent progression of the damage into arthritis.
Anatomy of Articular Cartilage
Articular cartilage is the smooth, shiny, white tissue covering the ends of bones that form a joint. Articular cartilage reduces friction when bones glide over each other, making the movements smooth and painless. It also acts as a shock-absorber to help prevent traumatic injuries to the bones.
Indications for Knee Cartilage Restoration
Knee cartilage restoration is indicated for patients with knee cartilage deterioration or damage as a result of:
- Repetitive use of the knee joint
- Trauma or injury
- Hormonal conditions, such as osteochondritis dissecans (OCD)
- Congenital deformities
Preparation for Knee Cartilage Restoration
Preoperative preparation for knee cartilage restoration will involve the following steps:
- A thorough examination by your doctor to check for any medical issues that need to be addressed prior to surgery.
- Depending on your medical history, social history, and age, routine blood work and imaging may be ordered for safely conducting surgery.
- You will be asked if you have any allergies to medications, anesthesia, or latex.
- You should inform your doctor of any medications, vitamins, or supplements that you may be taking.
- You should refrain from medications or supplements such as blood thinners, aspirin, or anti-inflammatory medicines for a week or two prior to surgery.
- You should refrain from alcohol or tobacco at least 24 hours prior to surgery.
- You should not consume any solids or liquids at least 8 hours prior to surgery.
- Arrange for someone to drive you home as you will not be able to drive yourself post surgery.
- A written consent will be obtained from you after the surgical procedure has been explained in detail.
Surgical Procedures for Knee Cartilage Restoration
Most cartilage restoration procedures can be performed arthroscopically, a minimally invasive surgery that involves making 3 small keyhole incisions around the knee joint using an arthroscope, a small flexible tube with a light and video camera at the end that enables your surgeon to view inside of the joints and perform surgery. In certain cases, open surgery may be required to access the affected area requiring longer incisions. Your surgeon will discuss the best surgical options for you based on your condition.
Usually, recovery from an arthroscopic procedure is much faster with minimal pain than a traditional, open surgery.
Some of the most common procedures for knee cartilage restoration include:
- Microfracture: In this method, numerous holes are created in the injured joint surface using a sharp tool. This procedure stimulates a healing response by creating a new blood supply which results in the growth of new cartilage.
- Drilling: In this method, a drilling instrument is used to create holes in the injured joint surface. Drilling holes creates blood supply and stimulates the growth of new cartilage. Although the method is similar to microfracture, it is less precise, and the heat produced during drilling may damage other tissues.
- Abrasion Arthroplasty: This procedure is similar to drilling, but a high-speed metal-like object is used to remove the damaged cartilage instead of drills or wires.
- Osteochondral Autograft Transplantation: Healthy cartilage tissue (graft) is taken from the bone that bears less weight and is transferred to the injured joint place. This method is used for smaller cartilage defects.
- Osteochondral Allograft Transplantation: A cartilage tissue (graft) is taken from a donor and transplanted to the site of the injury. Allograft technique is recommended if a larger part of the cartilage is damaged.
- Autologous Chondrocyte Implantation: In this method, a piece of healthy cartilage from another site is removed using an arthroscopic technique and is cultured in the laboratory. Cultured cells form a larger patch which is then implanted in the damaged part by open surgery.
Postoperative Care Instructions and Recovery
In general, postoperative care and recovery after knee cartilage restoration involve the following:
- You will be transferred to the recovery area to be monitored until you are awake from the anesthesia.
- Your nurse will monitor your blood oxygen level and other vital signs as you recover.
- You will be placed on crutches for the first few weeks with instructions on restricted weight-bearing. You are encouraged to walk with assistance as frequently as possible to prevent blood clots.
- Use of a continuous passive motion machine (CPM) at home is advised during the first few weeks to aid in the constant movement of the joint under a controlled range of motion.
- You are advised to keep your leg elevated while resting to prevent swelling and pain.
- You will notice some pain and discomfort in the knee area. Medications will be provided for comfort.
- Physical therapy and range of motion exercises are advised to restore mobility and strengthen the joints and muscles.
- Anti-nausea medications will be prescribed as needed for discomfort associated with anesthesia.
- You should keep your surgical site clean and dry for at least 48 hours. Instructions on surgical site care and bathing will be provided.
- Refrain from smoking as it can negatively affect the healing process.
- Eating a healthy diet rich in vitamin D is strongly advised to promote healing and a faster recovery.
- Refrain from strenuous activities or lifting heavy objects for the first couple of months. Gradual increase in activities over a period of time is recommended.
- You will be able to return to your normal activities in a month or two; however, return to sports may take 4 to 6 months.
- A follow-up appointment will be scheduled to monitor your progress.
Risks and Complications of Knee Cartilage Restoration
Knee cartilage restoration is a relatively safe procedure; however, as with any surgery, there are risks and complications that could occur, such as:
- Post-operative bleeding
- Blood clots (deep vein thrombosis)
- Infection
- Stiffness of the joint
- Numbness around the incisions
- Injury to vessels, nerves, or healthy cartilage
- Allergic response
- Failure of the graft
- Loosening of the graft
Related Topics
- Knee Arthroscopy
- ACL Reconstruction
- PCL Reconstruction
- LCL Reconstruction
- MCL Reconstruction
- LPFL Reconstruction
- Meniscal Surgery
- Partial Meniscectomy
- Medial Patellofemoral Ligament Reconstruction
- Knee Osteotomy
- Knee Cartilage Restoration
- Autologous Chondrocyte Implantation
- Osteochondral Allograft
- Osteochondral Autograft
- Patellar Tendon Repair
- Quadriceps Tendon Repair
- Meniscectomy
- Prior Meniscectomy
- Knee Fracture Surgery
- Multiligament Reconstruction of the Knee
- Posterolateral Corner (PLC) Reconstruction
- Revision Knee Ligament Reconstruction
- Mosaicplasty
- Posterolateral Corner Reconstruction
- Patellofemoral Realignment
- Failed Anterior Cruciate Ligament (ACL) Reconstruction
- Cartilage Microfracture
- Distal Realignment Procedures
- High Tibial Osteotomy
- Tibial Tubercle Osteotomy
- Distal Femoral Osteotomy
- Hamstring Autograft
- Hamstring Allograft
- Physeal Sparing Reconstruction of the Anterior Cruciate Ligament
- Bone-Patellar Tendon-Bone (BPTB) Allograft
- Bone-Patellar Tendon-Bone (BPTB) Autograft
- Viscosupplementation
- Intraarticluar Knee Injection
- Quadriceps Tendon Autograft for ACL Reconstruction
